Last updated 02.23.2026
Can you get dental implants with other health conditions? What to know
Many people with common health conditions may still be candidates for dental implants. This guide explains how diabetes, osteoporosis/bisphosphonates, and bone loss may affect planning.

If you’ve been told you have bone loss, diabetes, osteoporosis, or take medications like Fosamax or Reclast, you may wonder whether dental implants are still an option.
The short answer: many people with common health conditions may still be candidates for dental implants. However, eligibility depends on how well a condition is managed, the medications involved, and how treatment is planned.
This guide explains how health history may affect dental implant treatment and what to expect during a consultation at ClearChoice Dental Implant Center.
Quick answer: many people with health conditions may still be candidates
Having a medical condition does not automatically disqualify you from dental implants. Candidacy typically depends on:
Overall health and condition stability
Medication use
Healing capacity
Individualized treatment planning
An evaluation that includes medical history review and imaging helps determine what options may be appropriate.
First, how dental implants work (and why health history matters)
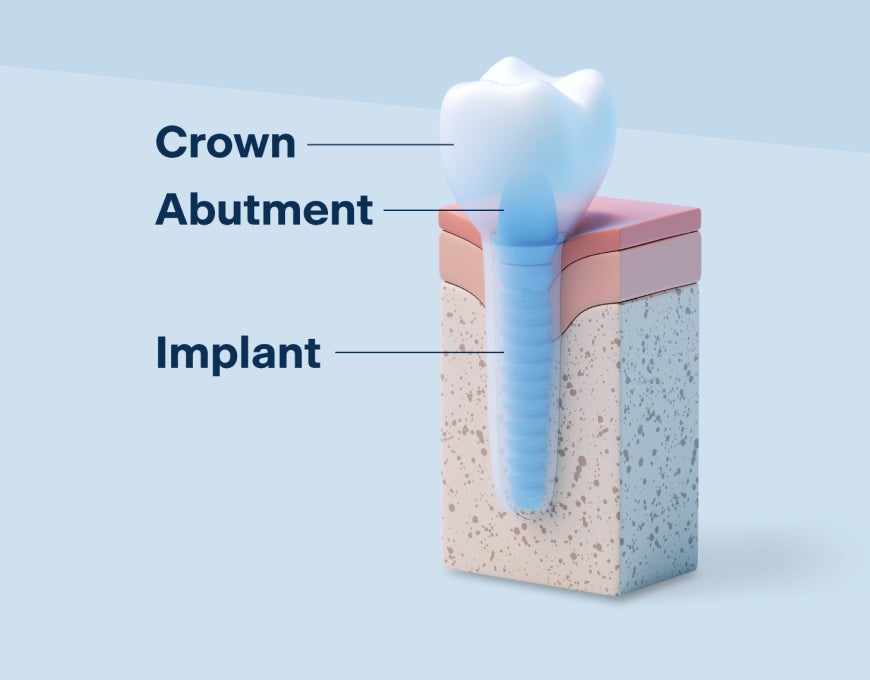
A dental implant restoration typically includes:
Implant post placed in the jawbone
Abutment (connector between the post and crown)
Crown or prosthetic restoration
For implants to succeed long term, the implant must integrate with the jawbone in a process called osseointegration. Systemic health conditions may affect:
Bone quality and quantity
Healing speed
Infection risk
Sedation or anesthesia planning (when applicable)
That’s why a full medical history is part of responsible treatment planning.
Health conditions that may affect implant planning
Below are common conditions patients ask about, along with how they may influence dental implant treatment.
Diabetes and dental implants
Many people search, can diabetics get dental implants?
The answer is often yes in many cases, people with diabetes may be candidates, particularly when blood sugar levels are well controlled.
Why it matters
Uncontrolled diabetes may affect healing and increase infection risk.
How planning may adapt
Coordination with your physician
Review of glycemic control
Careful monitoring during healing
Reinforced hygiene and follow-up guidance
Questions to ask
How does my current A1C level affect planning?
Are there additional healing considerations in my case?
Osteoporosis and dental implants
Osteoporosis affects bone density throughout the body, including the jaw.
Why it matters
Bone quality is an important factor in implant stability.
How planning may adapt
Osteoporosis alone does not automatically rule out implants. Evaluation of bone density in the jaw and overall oral health helps determine suitability.
Each case is individualized.
Bisphosphonates (Fosamax, Reclast) and dental implants
Patients frequently search terms like dental implants and Fosamax, Reclast and dental implants, or bisphosphonates and dental implants.
Bisphosphonates are medications commonly used to treat osteoporosis and other bone conditions.
Why it matters
These medications may affect bone turnover and healing.
How planning may adapt
Coordination with your prescribing physician may be recommended
Risk assessment based on dosage, duration, and route of administration (oral vs. IV)
Individualized evaluation of oral and bone health
Patients should never stop prescribed medications without guidance from their physician.
Bone loss and dental implants
One of the most common concerns is dental implants with bone loss or can you get dental implants with bone loss?
Why bone loss happens
Gum disease results in bone loss around teeth, and is a common reason that people lose their teeth. In addition, bone changes may occur after tooth loss because the jawbone no longer receives stimulation from natural tooth roots.
What this means for treatment
Depending on how much bone is missing, no special consideration for implant placement may be needed. In other cases, bone grafting may be discussed to help support implant placement. What causes bone loss around dental implants?
Bone loss around implants may be associated with:
Bite forces or grinding
Inconsistent maintenance
General health factors
Regular follow-up and hygiene are important for long-term support.

Other common conditions patients ask about
While bone loss and diabetes are among the most searched topics, other health considerations often come up.
Heart conditions or blood thinners
Treatment planning may include coordination with your physician. Medication adjustments should only occur under medical guidance.
Autoimmune conditions or immune-suppressing therapies
Risk assessment is individualized and may include additional precautions.
Smoking or nicotine use
Smoking may affect healing and implant success. Many providers recommend reducing or stopping use before and after treatment.
Sleep apnea or CPAP use
These may influence oral appliance planning or coordination of care.
Cancer history or radiation
Prior radiation to the head and neck may require specialized planning and referral coordination.
What to expect at a ClearChoice Dental Implant Center consultation
If you have a health condition, your consultation will focus on comprehensive planning. You can expect:
Detailed review of medical history and medications
Imaging to evaluate bone structure
Discussion of goals and timeline
Coordinated planning between surgical and restorative phases
Long-term maintenance guidance
Third-party financing options may be available for qualified applicants.
ClearChoice Dental Implant Center emphasizes education, coordination, and individualized care rather than one-size-fits-all treatment.
Questions to ask your provider if you have health conditions
If you’re considering dental implants, consider asking:
How does my condition affect healing or planning?
Do you coordinate with my physician if needed?
What is the maintenance plan after treatment?
What risks are possible in my case, and how are they managed?
If I have bone loss, what options may be considered?
FAQs: dental implants with health conditions
Can you get dental implants with bone loss?
In some cases, yes. Bone grafting or alternative planning strategies may be discussed depending on your jaw anatomy and health factors.
Can diabetics get dental implants?
Many people with well-controlled diabetes may be candidates. Evaluation and coordination with a physician may be part of planning.
Can you get dental implants if you have osteoporosis?
Osteoporosis does not automatically prevent implant treatment. Bone quality and overall health are evaluated individually.
Do Fosamax or Reclast affect dental implant treatment?
Bisphosphonate medications may influence planning and healing considerations. Coordination with your prescribing physician may be recommended.
What causes bone loss around dental implants?
Bone loss may be associated with gum inflammation, bite forces, systemic health factors, or inconsistent maintenance. Regular follow-up is important.
How long can dental implants last?
Dental implants are implants that can last a lifetime with proper care. However, restorations may require maintenance or replacement over time.
The bottom line
Having a health condition does not automatically mean you cannot receive dental implants. Many people with diabetes, osteoporosis, or bone loss may still be candidates when treatment is thoughtfully planned. A consultation at ClearChoice Dental Implant Center provides an opportunity to review your health history, imaging, and goals so you can understand your options and move forward with clarity.



